Diabetes
The content of this chapter is largely taken from Wikipedia
Content is incomplete and may be incorrect. |
Diabetes mellitus, or simply diabetes, is a group of metabolic diseases in which a person has high blood sugar, either because the pancreas does not produce enough insulin, or because cells do not respond to the insulin that is produced.[1] This high blood sugar produces the classical symptoms of polyuria (frequent urination), polydipsia (increased thirst) and polyphagia (increased hunger).
There are three main types of diabetes mellitus (DM).
- Type 1 DM results from the body's failure to produce insulin, and presently requires the person to inject insulin or wear an insulin pump. This form was previously referred to as insulin-dependent diabetes mellitus (IDDM) or juvenile diabetes.
- Type 2 DM results from insulin resistance, a condition in which cells fail to use insulin properly, sometimes combined with an absolute insulin deficiency. This form was previously referred to as non insulin-dependent diabetes mellitus (NIDDM) or adult-onset diabetes.
- The third main form, gestational diabetes occurs when pregnant women without a previous diagnosis of diabetes develop a high blood glucose level. It may precede development of type 2 DM.
Other forms of diabetes mellitus include congenital diabetes, which is due to genetic defects of insulin secretion, cystic fibrosis-related diabetes, steroid diabetes induced by high doses of glucocorticoids, and several forms of monogenic diabetes.
All forms of diabetes have been treatable since insulin became available in 1921, and type 2 diabetes may be controlled with medications. Both types 1 and 2 are chronic conditions that cannot be cured. Pancreas transplants have been tried with limited success in type 1 DM; gastric bypass surgery has been successful in many with morbid obesity and type 2 DM. Gestational diabetes usually resolves after delivery. Diabetes without proper treatments can cause many complications. Acute complications include hypoglycemia, diabetic ketoacidosis, or nonketotic hyperosmolar coma. Serious long-term complications include cardiovascular disease, chronic renal failure, and diabetic retinopathy (retinal damage). Adequate treatment of diabetes is thus important, as well as blood pressure control and lifestyle factors such as smoking cessation and maintaining a healthy body weight.
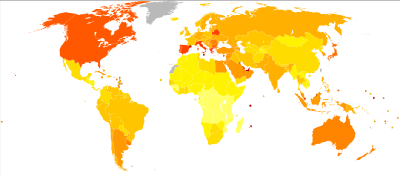
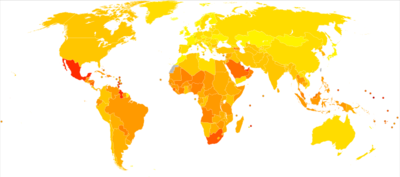
Globally, as of 2012, an estimated 346 million people have type 2 diabetes.[2]
Classification
| Comparison of type 1 and 2 diabetes[3] | ||
|---|---|---|
| Feature | Type 1 diabetes | Type 2 diabetes |
| Onset | Sudden | Gradual |
| Age at onset | Mostly in children | Mostly in adults |
| Body habitus | Thin or normal[4] | Often obese |
| Ketoacidosis | Common | Rare |
| Autoantibodies | Usually present | Absent |
| Endogenous insulin | Low or absent | Normal, decreased or increased |
| Concordance in identical twins | 50% | 90% |
| Prevalence | ~10% | ~90% |
Diabetes mellitus is classified into four broad categories: Type 1, Type 2, gestational diabetes and other specific types.[1] The other specific types are a collection of a few dozen individual causes.[1] The term diabetes, without qualification, usually refers to diabetes mellitus. The rare disease diabetes insipidus has similar symptoms as diabetes mellitus, but without disturbances in the sugar metabolism (insipidus means without taste in Latin).
The term type 1 diabetes has replaced several former terms, including childhood-onset diabetes, juvenile diabetes, and insulin-dependent diabetes mellitus (IDDM). Likewise, the term type 2 diabetes has replaced several former terms, including adult-onset diabetes, obesity-related diabetes, and noninsulin-dependent diabetes mellitus (NIDDM). Beyond these two types, there is no agreed-upon standard nomenclature.
Type 1 diabetes
Type 1 diabetes mellitus is characterized by loss of the insulin-producing beta cells of the islets of Langerhans in the pancreas, leading to insulin deficiency. This type can be further classified as immune-mediated or idiopathic. The majority of type 1 diabetes is of the immune-mediated nature, in which beta cell loss is a T-cell-mediated autoimmune attack.[5] There is no known preventive measure against Type 1 diabetes, which causes approximately 10% of diabetes mellitus cases in North America and Europe. Most affected people are otherwise healthy and of a healthy weight when onset occurs. Sensitivity and responsiveness to insulin are usually normal, especially in the early stages. Type 1 diabetes can affect children or adults, but was traditionally termed juvenile diabetes because a majority of these diabetes cases were in children.
Brittle diabetes, also known as unstable diabetes or labile diabetes, is a term that was traditionally used to describe to dramatic and recurrent swings in glucose levels, often occurring for no apparent reason in insulin-dependent diabetes. This term, however, has no biologic basis and should not be used.[6] There are many reasons for Type 1 diabetes to be accompanied by irregular and unpredictable hyperglycemias, frequently with ketosis, and sometimes serious hypoglycemias, including an impaired counterregulatory response to hypoglycemia, occult infection, gastroparesis (which leads to erratic absorption of dietary carbohydrates), and endocrinopathies (e.g., Addison's disease).[6] These phenomena are believed to occur no more frequently than in 1% to 2% of persons with Type 1 diabetes.[7]
Type 2 diabetes
Type 2 diabetes mellitus is characterized by insulin resistance, which may be combined with relatively reduced insulin secretion.[1] The defective responsiveness of body tissues to insulin is believed to involve the insulin receptor. However, the specific defects are not known. Diabetes mellitus cases due to a known defect are classified separately. Type 2 diabetes is the most common type.
In the early stage of Type 2, the predominant abnormality is reduced insulin sensitivity. At this stage, hyperglycemia can be reversed by a variety of measures and medications that improve insulin sensitivity or reduce glucose production by the liver.
Gestational diabetes
Gestational diabetes mellitus (GDM) resembles Type 2 diabetes in several respects, involving a combination of relatively inadequate insulin secretion and responsiveness. It occurs in about 2%–5% of all pregnancies and may improve or disappear after delivery. Gestational diabetes is fully treatable, but requires careful medical supervision throughout the pregnancy. About 20%–50% of affected women develop Type 2 diabetes later in life.
Though it may be transient, untreated gestational diabetes can damage the health of the fetus or mother. Risks to the baby include macrosomia (high birth weight), congenital cardiac and central nervous system anomalies, and skeletal muscle malformations. Increased fetal insulin may inhibit fetal surfactant production and cause respiratory distress syndrome. Hyperbilirubinemia may result from red blood cell destruction. In severe cases, perinatal death may occur, most commonly as a result of poor placental perfusion due to vascular impairment. Labor induction may be indicated with decreased placental function. A Caesarean section may be performed if there is marked fetal distress or an increased risk of injury associated with macrosomia, such as shoulder dystocia.
A 2008 study completed in the U.S. found the number of American women entering pregnancy with pre-existing diabetes is increasing. In fact, the rate of diabetes in expectant mothers has more than doubled in the past six years.[8] This is particularly problematic as diabetes raises the risk of complications during pregnancy, as well as increasing the potential for the children of diabetic mothers to become diabetic in the future.
Other types
Prediabetes indicates a condition that occurs when a person's blood glucose levels are higher than normal but not high enough for a diagnosis of Type 2 DM. Many people destined to develop Type 2 DM spend many years in a state of prediabetes which has been termed America's largest healthcare epidemic.[9][10]
Latent autoimmune diabetes of adults (LADA) is a condition in which Type 1 DM develops in adults. Adults with LADA are frequently initially misdiagnosed as having Type 2 DM, based on age rather than etiology.
Some cases of diabetes are caused by the body's tissue receptors not responding to insulin (even when insulin levels are normal, which is what separates it from Type 2 diabetes); this form is very uncommon. Genetic mutations (autosomal or mitochondrial) can lead to defects in beta cell function. Abnormal insulin action may also have been genetically determined in some cases. Any disease that causes extensive damage to the pancreas may lead to diabetes (for example, chronic pancreatitis and cystic fibrosis). Diseases associated with excessive secretion of insulin-antagonistic hormones can cause diabetes (which is typically resolved once the hormone excess is removed). Many drugs impair insulin secretion and some toxins damage pancreatic beta cells. The ICD-10 (1992) diagnostic entity, malnutrition-related diabetes mellitus (MRDM or MMDM, ICD-10 code E12), was deprecated by the World Health Organization when the current taxonomy was introduced in 1999.[10]
Signs and symptoms
The classic symptoms of untreated diabetes are loss of weight, polyuria (frequent urination), polydipsia (increased thirst) and polyphagia (increased hunger).[11] Symptoms may develop rapidly (weeks or months) in Type 1 diabetes, while they usually develop much more slowly and may be subtle or absent in Type 2 diabetes.
Prolonged high blood glucose can cause glucose absorption in the lens of the eye, which leads to changes in its shape, resulting in vision changes. Blurred vision is a common complaint leading to a diabetes diagnosis; Type 1 should always be suspected in cases of rapid vision change, whereas with Type 2 change is generally more gradual, but should still be suspected. A number of skin rashes that can occur in diabetes are collectively known as diabetic dermadromes.
Diabetic emergencies
People (usually with Type 1 diabetes) may also present with diabetic ketoacidosis, a state of metabolic dysregulation characterized by the smell of acetone, a rapid, deep breathing known as Kussmaul breathing, nausea, vomiting and abdominal pain, and altered states of consciousness.
A rare but equally severe possibility is hyperosmolar nonketotic state, which is more common in Type 2 diabetes and is mainly the result of dehydration.
Complications
All forms of diabetes increase the risk of long-term complications. These typically develop after many years (10–20), but may be the first symptom in those who have otherwise not received a diagnosis before that time. The major long-term complications relate to damage to blood vessels. Diabetes doubles the risk of cardiovascular disease.[12] The main macrovascular diseases (related to atherosclerosis of larger arteries) are ischemic heart disease (angina and myocardial infarction), stroke and peripheral vascular disease.
Diabetes also damages the capillaries (causes microangiopathy).[13] Diabetic retinopathy, which affects blood vessel formation in the retina of the eye, can lead to visual symptoms, reduced vision, and potentially blindness. Diabetic nephropathy, the impact of diabetes on the kidneys, can lead to scarring changes in the kidney tissue, loss of small or progressively larger amounts of protein in the urine, and eventually chronic kidney disease requiring dialysis. Diabetic neuropathy is the impact of diabetes on the nervous system, most commonly causing numbness, tingling and pain in the feet and also increasing the risk of skin damage due to altered sensation. Together with vascular disease in the legs, neuropathy contributes to the risk of diabetes-related foot problems (such as diabetic foot ulcers) that can be difficult to treat and occasionally require amputation.
Causes
The cause of diabetes depends on the type.
Type 1 diabetes is partly inherited, and then triggered by certain infections, with some evidence pointing at Coxsackie B4 virus. A genetic element in individual susceptibility to some of these triggers has been traced to particular HLA (Human leukocyte antigen) genotypes (i.e., the genetic self identifiers relied upon by the immune system). However, even in those who have inherited the susceptibility, Type 1 DM seems to require an environmental trigger. The onset of Type 1 diabetes is unrelated to lifestyle.
Type 2 diabetes is due primarily to lifestyle factors and genetics.[14]
| The following is a comprehensive list of other causes of diabetes:[15] | |
|---|---|
|
|
Pathophysiology
Insulin is the principal hormone that regulates uptake of glucose from the blood into most cells (primarily muscle and fat cells, but not central nervous system cells). Therefore, deficiency of insulin or the insensitivity of its receptors plays a central role in all forms of diabetes mellitus.
Humans are capable of digesting some carbohydrates, in particular those most common in food; starch, and some disaccharides such as sucrose, are converted within a few hours to simpler forms, most notably the monosaccharide glucose, the principal carbohydrate energy source used by the body. The rest are passed on for processing by gut flora largely in the colon. Insulin is released into the blood by beta cells (ß-cells), found in the islets of Langerhans in the pancreas, in response to rising levels of blood glucose, typically after eating. Insulin is used by about two-thirds of the body's cells to absorb glucose from the blood for use as fuel, for conversion to other needed molecules, or for storage.
Insulin is also the principal control signal for conversion of glucose to glycogen for internal storage in liver and muscle cells. Lowered glucose levels result both in the reduced release of insulin from the ß-cells and in the reverse conversion of glycogen to glucose when glucose levels fall. This is mainly controlled by the hormone glucagon, which acts in the opposite manner to insulin. Glucose thus forcibly produced from internal liver cell stores (as glycogen) re-enters the bloodstream; muscle cells lack the necessary export mechanism. Normally, liver cells do this when the level of insulin is low (which normally correlates with low levels of blood glucose).
Higher insulin levels increase some anabolic (building up) processes, such as cell growth and duplication, protein synthesis, and fat storage. Insulin (or its lack) is the principal signal in converting many of the bi-directional processes of metabolism from a catabolic to an anabolic direction, and vice versa. In particular, a low insulin level is the trigger for entering or leaving ketosis (the fat-burning metabolic phase).
If the amount of insulin available is insufficient, if cells respond poorly to the effects of insulin (insulin insensitivity or resistance), or if the insulin itself is defective, then glucose will not have its usual effect, so it will not be absorbed properly by those body cells that require it, nor will it be stored appropriately in the liver and muscles. The net effect is persistent high levels of blood glucose, poor protein synthesis, and other metabolic derangements, such as acidosis.
When the glucose concentration in the blood is raised to about 9-10 mmol/L (except certain conditions, such as pregnancy), beyond its renal threshold (i.e. when glucose level surpasses the transport maximum of glucose reabsorption), reabsorption of glucose in the proximal renal tubuli is incomplete, and part of the glucose remains in the urine (glycosuria). This increases the osmotic pressure of the urine and inhibits reabsorption of water by the kidney, resulting in increased urine production (polyuria) and increased fluid loss. Lost blood volume will be replaced osmotically from water held in body cells and other body compartments, causing dehydration and increased thirst.
Diagnosis
| Diabetes diagnostic criteria[17][18] | |||
|---|---|---|---|
| Condition | 2 Hour Glucose | Fasting glucose | HbA1c |
| mmol/l(mg/dl) | mmol/l(mg/dl) | % | |
| Normal | <7.8 (<140) | <6.1 (<110) | <6.0 |
| Impaired fasting glycaemia | <7.8 (<140) | ≥ 6.1(≥110) & <7.0(<126) | 6.0–6.4 |
| Impaired glucose tolerance | ≥7.8 (≥140) | <7.0 (<126) | 6.0–6.4 |
| Diabetes mellitus | ≥11.1 (≥200) | ≥7.0 (≥126) | ≥6.5 |
Diabetes mellitus is characterized by recurrent or persistent hyperglycemia, and is diagnosed by demonstrating any one of the following:[10]
- Fasting plasma glucose level ≥7.0 mmol/l (126 mg/dl)
- Plasma glucose ≥11.1 mmol/l (200 mg/dL) two hours after a 75g oral glucose load as in a glucose tolerance test
- Symptoms of hyperglycemia and casual plasma glucose ≥11.1 mmol/l (200 mg/dl)
- Glycated hemoglobin (Hb A1C) ≥6.5%[19]
A positive result, in the absence of unequivocal hyperglycemia, should be confirmed by a repeat of any of the above methods on a different day. It is preferable to measure a fasting glucose level because of the ease of measurement and the considerable time commitment of formal glucose tolerance testing, which takes two hours to complete and offers no prognostic advantage over the fasting test.[20] According to the current definition, two fasting glucose measurements above 126 mg/dl (7.0 mmol/l) is considered diagnostic for diabetes mellitus.
People with fasting glucose levels from 110 to 125 mg/dl (6.1 to 6.9 mmol/l) are considered to have impaired fasting glucose.[21] Patients with plasma glucose at or above 140 mg/dL (7.8 mmol/L), but not over 200 mg/dL (11.1 mmol/L), two hours after a 75 g oral glucose load are considered to have impaired glucose tolerance. Of these two prediabetic states, the latter in particular is a major risk factor for progression to full-blown diabetes mellitus, as well as cardiovascular disease.[22]
Glycated hemoglobin is better than fasting glucose for determining risks of cardiovascular disease and death from any cause.[23]
Management
Diabetes mellitus is a chronic disease which cannot be cured except in very specific situations. Management concentrates on keeping blood sugar levels as close to normal (euglycemia) as possible, without causing hypoglycemia. This can usually be accomplished with diet, exercise, and use of appropriate medications (insulin in the case of Type 1 diabetes, oral medications, as well as possibly insulin, in Type 2 diabetes).
Patient education, understanding, and participation is vital, since the complications of diabetes are far less common and less severe in people who have well-managed blood sugar levels.[24][25] The goal of treatment is an HbA1C level of 6.5%, but should not be lower than that, and may be set higher.[26] Attention is also paid to other health problems that may accelerate the deleterious effects of diabetes. These include smoking, elevated cholesterol levels, obesity, high blood pressure, and lack of regular exercise.[26]
Lifestyle
There are roles for patient education, dietetic support, sensible exercise, with the goal of keeping both short-term and long-term blood glucose levels within acceptable bounds. In addition, given the associated higher risks of cardiovascular disease, lifestyle modifications are recommended to control blood pressure.[27]
Medications
The following table compares some common anti-diabetic agents, generalizing classes, although there may be substantial variation in individual drugs of each class. When the table makes a comparison such as "lower risk" or "more convenient" the comparison is with the other drugs on the table.
| Comparison of anti-diabetic medication[28][29][30][31] | |||
|---|---|---|---|
| Agent[29][30][31] | Mechanism[32] | Advantages[29][30][31] | Disadvantages[29][30][31] |
| Sulfonylurea (glyburide, glimepiride, glipizide) | Stimulating insulin release by pancreatic beta cells by inhibiting the KATP channel |
|
|
| Metformin | Acts on liver to cause decrease in insulin resistance |
|
|
| Alpha-glucosidase inhibitor (acarbose, miglitol) | Reduces glucose absorbance by acting on small intestine to cause decrease in production of enzymes needed to digest carbohydrates |
|
|
| Thiazolidinediones (Actos, Avandia) | Reduce insulin resistance by activating (Peroxisome proliferator-activated receptor gamma) PPAR-γ in fat and muscle |
|
|
Most anti-diabetic agents are contraindicated in pregnancy, in which insulin is preferred.[29]
Oral medications
Metformin is generally recommended as a first line treatment for Type 2 diabetes, as there is good evidence that it decreases mortality.[33] Routine use of aspirin, however, has not been found to improve outcomes in uncomplicated diabetes.[34]
Insulin
Type 1 diabetes is typically treated with a combinations of regular and NPH insulin, or synthetic insulin analogs. When insulin is used in Type 2 diabetes, a long-acting formulation is usually added initially, while continuing oral medications.[33] Doses of insulin are then increased to effect.[33]
Support
In countries using a general practitioner system, such as the United Kingdom, care may take place mainly outside hospitals, with hospital-based specialist care used only in case of complications, difficult blood sugar control, or research projects. In other circumstances, general practitioners and specialists share care of a patient in a team approach. Optometrists, podiatrists/chiropodists, dietitians, Physical therapy|physiotherapists, nursing specialists (e.g., diabetic specialist nurses), nurse practitioners, or certified diabetes educators, may jointly provide multidisciplinary expertise. Home telehealth support can be an effective management technique.[35]
Epidemiology
Globally, as of 2010, an estimated 285 million people had diabetes, with Type 2 making up about 90% of the cases.[3] Its incidence is increasing rapidly, and by 2030, this number is estimated to almost double.[36] Diabetes mellitus occurs throughout the world, but is more common (especially Type 2) in the more developed countries. The greatest increase in prevalence is, however, expected to occur in Asia and Africa, where most patients will probably be found by 2030.[36] The increase in incidence in developing countries follows the trend of urbanization and lifestyle changes, perhaps most importantly a Western-style diet. This has suggested an environmental (i.e., dietary) effect, but there is little understanding of the mechanism(s) at present, though there is much speculation, some of it most compellingly presented.[36]
Australia
Indigenous populations in first world countries have a higher prevalence and increasing incidence of diabetes than their corresponding nonindigenous populations. In Australia, the age-standardised prevalence of self-reported diabetes in indigenous Australians is almost four times that of nonindigenous Australians.[37] Preventative community health programs, such as Sugar Man (diabetes education), are showing some success in tackling this problem.
China
Almost one Chinese adult in ten has diabetes. A 2010 study estimated that more than 92 million Chinese adults have the disease, with another 150 million showing early symptoms.[38] The incidence of the disease is increasing rapidly; a 2009 study found a 30% increase in 7 years.[39]
India
India has more diabetics than any other country in the world, according to the International Diabetes Foundation,[40] although more recent data suggest that China has even more.[38] The disease affects more than 50 million Indians - 7.1% of the nation's adults - and kills about 1 million Indians a year.[40] The average age on onset is 42.5 years.[40] The high incidence is attributed to a combination of genetic susceptibility plus adoption of a high-calorie, low-activity lifestyle by India's growing middle class.[41]
United Kingdom
About 3.8 million people in the United Kingdom have diabetes mellitus, but the charity Diabetes U.K. have made predictions that that could become high as 6.2 million by 2035/2036. Diabetes U.K. have also predicted that the National Health Service could be spending as much as 16.9 billion pounds on diabetes mellitus by 2035, a figure that means the NHS could be spending as much as 17% of its budget on diabetes treatment by 2035.[42][43][44]
United States
For at least 20 years, diabetes rates in North America have been increasing substantially. In 2010, nearly 26 million people have diabetes in the United States, of whom 7 million people remain undiagnosed. Another 57 million people are estimated to have prediabetes.[45][46]
The Centers for Disease Control and Prevention (CDC) has termed the change an epidemic.[47] The National Diabetes Information Clearinghouse estimates diabetes costs $132 billion in the United States alone every year. About 5%–10% of diabetes cases in North America are Type 1, with the rest being Type 2. The fraction of Type 1 in other parts of the world differs. Most of this difference is not currently understood. The American Diabetes Association (ADA) cites the 2003 assessment of the National Center for Chronic Disease Prevention and Health Promotion (Centers for Disease Control and Prevention) that one in three Americans born after 2000 will develop diabetes in their lifetimes.[48][49]
According to the ADA, about 18.3% (8.6 million) of Americans age 60 and older have diabetes.[50] Diabetes mellitus prevalence increases with age, and the numbers of older persons with diabetes are expected to grow as the elderly population increases in number. The National Health and Nutrition Examination Survey (NHANES III) demonstrated, in the population over 65 years old, 18% to 20% have diabetes, with 40% having either diabetes or its precursor form of impaired glucose tolerance.[51]
References
Error fetching PMID 406527:
Error fetching PMID 18223030:
Error fetching PMID 18977856:
Error fetching PMID 20609967:
Error fetching PMID 21791495:
Error fetching PMID 19032965:
Error fetching PMID 20167359:
Error fetching PMID 20194231:
Error fetching PMID 11473076:
Error fetching PMID 20200384:
Error fetching PMID 16371630:
Error fetching PMID 7887548:
Error fetching PMID 10938049:
Error fetching PMID 19145963:
Error fetching PMID 20508233:
Error fetching PMID 19531058:
Error fetching PMID 15111519:
Error fetching PMID 14532317:
Error fetching PMID 9571335:
-
Shoback, edited by David G. Gardner, Dolores (2011). Greenspan's basic & clinical endocrinology (9th ed.). New York: McGraw-Hill Medical. pp. Chapter 17. ISBN 0-07-162243-8.
-
Williams textbook of endocrinology (12th ed.). Philadelphia: Elsevier/Saunders. pp. 1371–1435. ISBN 978-1-4377-0324-5.
-
Lambert, P.; Bingley, P. J. (2002). What is Type 1 Diabetes?. Medicine 30: 1–5. doi:10.1383/medc.30.1.1.28264. Diabetes Symptoms edit
- Error fetching PMID 17429082:
-
Diabetes Mellitus (DM): Diabetes Mellitus and Disorders of Carbohydrate Metabolism: Merck Manual Professional. Merck Publishing. April 2010. Retrieved 2010-07-30.
- Error fetching PMID 406527:
- Error fetching PMID 18223030:
-
Handelsman Y, MD. A Doctor's Diagnosis: Prediabetes. Power of Prevention 1 (2).
-
Definition, Diagnosis and Classification of Diabetes Mellitus and its Complications (PDF). World Health Organisation. 1999.
- Error fetching PMID 18977856:
- Error fetching PMID 20609967:
- Error fetching PMID 21791495:
- Error fetching PMID 19032965:
-
Unless otherwise specified, reference is: Table 20-5 in Mitchell, Richard Sheppard; Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson. Robbins Basic Pathology. Philadelphia: Saunders. ISBN 1-4160-2973-7. 8th edition.
- Error fetching PMID 20167359:
-
Definition and diagnosis of diabetes mellitus and intermediate hyperglycemia: report of a WHO/IDF consultation. Geneva: World Health Organization. 2006. p. 21. ISBN 978-92-4-159493-6.
- Error fetching PMID 20194231:
-
Diabetes Care January 2010. American Diabetes Association. Retrieved 2010-01-29.
- Error fetching PMID 11473076:
-
Definition and diagnosis of diabetes mellitus and intermediate hyperglycemia : report of a WHO/IDF consultation. World Health Organization. 2006. p. 21. ISBN 978-92-4-159493-6.
-
Santaguida PL, Balion C, Hunt D, Morrison K, Gerstein H, Raina P, Booker L, Yazdi H. Diagnosis, Prognosis, and Treatment of Impaired Glucose Tolerance and Impaired Fasting Glucose. Summary of Evidence Report/Technology Assessment, No. 128. Agency for Healthcare Research and Quality. Retrieved 2008-07-20.
- Error fetching PMID 20200384:
- Error fetching PMID 16371630:
- Error fetching PMID 7887548:
-
National Institute for Health and Clinical Excellence. Clinical guideline 66: Type 2 diabetes. London, 2008.
- Error fetching PMID 10938049:
- Error fetching PMID 19145963:
- Error fetching PMID 20508233:
- Error fetching PMID 19531058:
- Error fetching PMID 15111519:
-
Australian Institute for Health and Welfare. Diabetes, an overview. Archived from the original on 2008-06-17. Retrieved 2008-06-23.
-
China faces 'diabetes epidemic', research suggests. BBC. March 25, 2010. Retrieved 8 June 2012.
-
Grens, Kerry (April 4, 2012). Diabetes continuing to spike in China. Reuters. Retrieved 8 June 2012.
-
Gale, Jason (November 7, 2010). India’s Diabetes Epidemic Cuts Down Millions Who Escape Poverty. Bloomberg. Retrieved 8 June 2012.
-
Kleinfield, N. R. (September 13, 2006). Modern Ways Open India’s Doors to Diabetes. New York Times. Retrieved 8 June 2012.
-
NHS spending on diabetes 'to reach £16.9 billion by 2035'. 2012-04-25. Retrieved 2012-04-26.
-
Number of Americans with Diabetes Rises to Nearly 26 Million (Press release). Centers for Disease Control and Prevention. 2011-01-26. Retrieved 2012-05-27.
-
National diabetes fact sheet: national estimates and general information on diabetes and prediabetes in the United States, 2011. Centers for Disease Control and Prevention. 2011. Retrieved 2012-05-31.
-
Diabetes Rates Rise Another 6 Percent in 1999 — January 26, 2001. Retrieved 2008-06-23.
- Error fetching PMID 14532317:
-
Total Prevalence of Diabetes & Pre-diabetes. American Diabetes Association. 2005. Archived from the original on 2006-02-08. Retrieved 2006-03-17.
-
Seniors and Diabetes. Elderly And Diabetes-Diabetes and Seniors. LifeMed Media. 2006. Retrieved 2007-05-14.
- Error fetching PMID 9571335:
-
Diabetes Blue Circle Symbol. International Diabetes Federation. 17 March 2006.
The content of this chapter is largely taken from Wikipedia
Content is incomplete and may be incorrect. |
Preamble
Diabetes (diabetes mellitus) is one of the metabolic diseases with higher blood sugar level, either due to the pancreatic beta cells do not produce enough insulin, or the cells do not respond to the insulin that is produced.[52] Its clinical symptoms include three polies: polyuria (frequent urination), polydipsia (increased thirst) and polyphagia (increased hunger).
Diabetes is categorized as three types in the clinic: Type 1 diabetes (T1D, diabetes mellitus 1, DM1) results from pancreatic beta cell destruction and thus fails to produce insulin, and is insulin dependent which relies on insulin injection, it is also named insulin-dependent diabetes mellitus (IDDM). Since T1D happens mostly in juveniles it is also called juvenile-onset diabetes. Type 2 diabetes (T2D, diabetes mellitus 2, DM2) results from the reason that the beta cells do not respond to insulin (insulin resistance), and it may co-exist with the situation of partially or fully insulin-dependent, which is also named non-insulin-dependent diabetes mellitus (NIDDM) or adult-onset diabetes. In some type 2 diabetes, concomitant insulin therapy may be necessary (IDDM2). The third type is gestational diabetes occurs while pregnancy.
| Comparison of type 1 and 2 diabetes[3] | ||
|---|---|---|
| Feature | Type 1 diabetes | Type 2 diabetes |
| Onset | Sudden | Gradual |
| Age at onset | Mostly in children | Mostly in adults |
| Body habitus | Thin or normal[4] | Often obese |
| Ketoacidosis | Common | Rare |
| Autoantibodies | Usually present | Absent |
| Endogenous insulin | Low or absent | Normal, decreased or increased |
| Concordance in identical twins | 50% | 90% |
| Prevalence | ~10% | ~90% |
There is no cure for diabetes currently except that most of the gestational diabetes disappears when the pregnancy is ended, but it is treatable. The current therapies are insulin, other non-curing medications, and pancreatic replacement therapies like pancreatic islet transplantations which have been applied to severe T1D cases successfully since 1980s’.[1]Since both T1D and T2D are chronic diseases and the progresses of modern medicine, acute complications like hypoglycemia and ketoacidosis are under well controlled, and thus chronic and long-term complications like chronic renal failure, and diabetic retinopathy, especially cardiovascular diseases (CVD), are drawing attentions.
| Basic treatment steps of diabetes: | |
|---|---|
| Step 1 | Educate the patient
Treat concomittant risk factors (e.g. hypertension, obesity, hyperlipidemia) start met metformine (500 mg 1 dd, max. 1000 mg 3 dd) start cholesterol lowering drug (e.g. simvastatine 40mg once daily) start ACE inhibitor if no hypertension but with microalbuminuria (e.g. enalapril 10-20mg once daily) |
| Step 2 | BMI <27: add sulfonylureumderivate (eg. tolbutamide 500 mg once daily, max. 1000 mg twice daily)
BMI =27: add sulfonylureumderivaat if no CVD or heart failure If CVD but no increased risk of heart failure add (pioglitazon 15 mg once daily, max. 45 mg once daily) |
| Step 3 | Add long acting insulin to oral treatment (stop pioglitazon if present) |
| Step 4a | NPH-insuline or mix-insuline twice daily |
| Step 4b | Insulin four times daily |
Case Report
Rick is a 56-year-old plumber of a local firm, and his friends called him stocky since he is 7’8” and 260 lbs. He is married and was diagnosed with type 2 diabetes 14 months ago. He used to smoke 10 cigarettes a day and is currently not smoking, but he continued to eat fatty fast food seven to ten times per week due to his flow of work.
He had followed lifestyle advice and lost some weight and was doing more exercises, but had now been diagnosed with hypertension (163/95 mmHg). His physician decided to offer Rick some treatments for his hypertension, and Rick attended for a further check-up 18 months after the diabetic diagnosis. It was found that Rick now has chest pain, and he had to start taking aspirin and a beta blocker.
Introduction
As per the World Health Organization (WHO), an estimated 347 million people world-wide have diabetes in 2012.[53] The number of deaths attributed to diabetes was previously estimated at just over 800,000. However, it has long been known that the number of deaths related to diabetes is considerably underestimated. With regarding the causes of death of diabetes, one important factor contributing the increased morbidity and mortality in diabetic individuals is the development of cardiovascular disease, one of the chronic complications of diabetes. Several studies have demonstrated that diabetic patients have a risk of death that is two to three times higher than that among people without diabetes.[3]
| The following is a comprehensive list of other causes of diabetes:[15] | |
|---|---|
|
|
Multiple epidemiologic studies have established diabetes as a major risk factor for the development of all manifestations of cardiovascular disease, including myocardial infarction, stroke, peripheral vascular disease, and heart failure,[4][5][6][7] and recent data suggest that the proportion of cardiovascular disease attributable to diabetes is increasing.[5] It is estimated that cardiovascular disease accounts for 65% of all deaths in persons with diabetes.[8] In a recent meta-analysis of nearly 700,000 people from 102 prospective studies, diabetes conferred an approximate two fold risk for coronary heart disease and stroke, independently from other conventional risk factors.[7] Thus, in order to reduce the health burden of diabetes, it is considered necessary to aggressively prevent and treat cardiovascular disease in these patients.
Diabetes and pre-diabetic glucose abnormalities
Type 1 diabetes is caused by the gradually decreasing of endogenous insulin production by pancreatic beta cells and thus loss of the control of blood glucose, whereas type 2 diabetes is caused by the rising blood glucose resulted from a combination of genetic predisposition, unhealthy diet, physical inactivity, and body weight-gain.[9] The higher than normal blood glucose level in both type 1 and type 2 diabetes results in pathophysiological processes, which are associated with the development of microvascular disease and atherosclerosis. Patients with diabetes are thus at a particularly high risk for cardiovascular, cerebrovascular, and peripheral artery disease.
Diabetes is characterized by recurrent or persistent hyperglycemia (high blood glucose), and is diagnosed by demonstrating any one of the following:[10]
- Fasting blood glucose level = 126 mg/dl (= 7.0 mmol/L)
- 2 hours glucose tolerance test: Plasma glucose = 200 mg/dL (= 11.1 mmol/L)
- HbA1C IFCC = 48 mmol/mol (6.5%)
A positive result should be confirmed by a repeat on a different day. People with fasting glucose levels from 110 to 125 mg/dl (6.1 to 7.0 mmol/L) are considered to have impaired fasting glucose.[11] People with blood glucose at 140 mg/dL ~ 200 mg/dL (7.8 ~ 11.1 mmol/L) as glucose tolerance test result are considered to have impaired glucose tolerance, which in particular is a major risk for progression to diabetes, as well as cardiovascular disease.[12] HbA1C (glycated hemoglobin), which is an indicator of average blood glucose level, is better than fasting glucose for determining risks of cardiovascular disease and death from any cause.[13] Measuring HbA1C assesses the effectiveness of therapy by monitoring long-term serum glucose regulation, and patients with diabetes who manage to keep their HbA1C level below 53 mmol/mol (7%) are considered to have good glycemic control.
Epidemiology and cardiovascular risk of diabetes
The age-specific prevalence of diabetes rises with age up to the seventh to eighth decades in both men and women.[14] The prevalence is less than 10% in subjects below the age of 60, and 10–20% between 60 ~ 69 years; 15–20% in the oldest groups have previously known diabetes; and a similar proportion have screen-detected asymptomatic diabetes. This suggests that the lifetime risk of diabetes in European people is 30–40%. The prevalence of impaired glucose tolerance increases linearly with age, but the prevalence of impaired fasting glycaemia does not. In middle aged people, the prevalence of impaired glucose homeostasis is about 15%, whereas it is 35–40% in the elderly. The prevalence of diabetes and impaired glucose tolerance defined by isolated post-load hyperglycemia is higher in women than in men, but the prevalence of diabetes and impaired fasting glucose diagnosed by isolated fasting hyperglycemia is higher in men than in women.
Several prospective studies have unequivocally confirmed that post-load hyperglycemia increases cardiovascular diseases morbidity and mortality, however, it remains to be demonstrated that lowering a high 2-hours post-load blood glucose will reduce the risk. Studies are underway but thus far data are scarce. A secondary endpoint analysis of the STOP-NIDDM (Study to Prevent Non-Insulin-Dependent Diabetes Mellitus) revealed statistically significant reductions in cardiovascular diseases event rates in impaired glucose tolerance subjects receiving acarbose compared with placebo.[15] Since acarbose specifically reduces post-prandial glucose excursions, this is the first demonstration that lowering post-prandial glucose and may lead to a reduction in cardiovascular diseases events, but it should be noted that the power in this analysis is low due to a small number of cases.
Identification of subjects at high risk for CVD
Predicting risk of cardiovascular disease in diabetics can be done with the risk score of the DECODE study. The Diabetes Epidemiology: Collaborative Analysis Of Diagnostic Criteria in Europe (DECODE) group developed a cardiovascular diseases risk score, which is presently the only one of its kind including impaired glucose tolerance or impaired fasting glucose in the risk function determination.[16] The large European DECODE study is a collaborative prospective study of 22 cohorts in Europe with baseline glucose measurements for 29714 subjects aged 30-89 years who were followed-up for 11 years, indicated that either fasting or 2-hours post-load blood glucose is an independent risk factor for all-cause and cardiovascular morbidity and mortality even in people without diagnosed diabetes.[17]
Predicting risk to develop diabetes is possible with the Finnish Diabetes Risk Score.[18] The Finnish Diabetes Risk Score predicts the 10 year risk for developing type 2 diabetes with 85% accuracy. It also detects asymptomatic diabetes and abnormal glucose tolerance with high reliability in other populations, which can be used as a self-administered test to screen subjects at high risk for type 2 diabetes, and can also be used in the general population and clinical practice to identify undetected type 2 diabetes, and the abnormal glucose tolerance. In addition, Finnish Diabetes Risk Score is a good predictor that can be used to predict coronary artery disease, stroke and total mortality.[19] Such a simple scoring system can be used to identify high-risk individuals. If under proper management, it can be applied to not only diabetes prevention, but also to cardiovascular diseases prevention.
Treatments to reduce cardiovascular risk
(Insert Table: ‘Treatment to reduce cardiovascular risk’, PMID17220161, p11) [38]
To reduce the risk of cardiovascular disease, the followings are needed to be considered: a) the prevention of the progression of diabetes; b) the prevention of cardiovascular disease by physical activity; and c) the treatments to reduce cardiovascular risk. With regarding the first treatment – the prevention of the progression of diabetes, clinical studies have demonstrated that effective lifestyle intervention strategies and drug treatments can prevent or at least delay the progression to type 2 diabetes in high-risk individuals. For instance, the Finnish Diabetes Prevention Study found that a 5% reduction in bodyweight, achieved through an intensive diet and exercise program was associated with a 58% reduction in the risk of developing type 2 diabetes in overweight subjects with impaired glucose tolerance;[20] and the US Diabetes Prevention Program found that lifestyle modification reduced the incidence of type 2 diabetes by 58% in overweight adults with impaired glucose tolerance.[21]
As the second treatment, the prevention of cardiovascular disease by physical activity, The International Diabetes Federation (European Region) have recommended physical activity for the prevention of cardiovascular disease complications among diabetic patients,[22] since studies found that physical activity was associated with reduced risk of cardiovascular disease, cardiovascular death, and total mortality in men with type 2 diabetes. People physically active at their work had a 40% lower cardiovascular mortality compared with people with lower physical activity at work. A high level of leisure-time physical activity like walking and walking pace was associated with a 33% drop in cardiovascular mortality, and moderate physical activity was linked to a 17% drop in cardiovascular mortality compared with the most sedentary group.[23]
To reduce cardiovascular risk in both type 1 and type 2 diabetes long-term hyperglycemia should be treated aggressively. These patients often have a combination of the major vascular risk factors known as the metablolic syndrome.[24][25] The additional treatment of metabolic syndrome is strongly based on non-pharmacological therapy including lifestyle changes, self-monitoring, and requires structured patient education including a heavy emphasis on smoking cessation, etc.[26][27][33] Specific recommendations include 30 min of physical activity for at least five times weekly, increase of fiber uptake to 30g daily, restriction of calorie intake to 1500 calorie daily, restriction of fat intake to 30–35% of total daily uptake, avoidance of trans-fats, and avoidance of liquid mono- and disaccharides. And the most importance of them, a tight glycemic control which will be described in the CAD treatment section.
CAD and diabetes
Case Report
Max is a 53 year old male administrator who had had high blood glucose for 12 months, and a random reading exceeds 342 mg/dL (18.9 mmol/L), blood glucose HBA1C 83.6 mmol/L (9.8%), normal blood pressure 136/92 mmHg on an office visit with a body mass index of 29. He started feeling a little tired recently and was getting up at night to urinate two to three times weekly. Max was eating as usual with no diabetes meal plan at this time, and had limited activities and rare exercise monthly. A few months ago, he got a myocardial infarction and was taking some cardiovascular and hypertensive medications. Max was trying to communicate with his physician and to search the internet to find out some effective solutions to reduce his risks of progression of his coronary artery disease and other cardiovascular complications.
Introduction
The most common cause of death in European diabetic adults is coronary artery disease (CAD). Studies have demonstrated that the risk is two to three times higher than that among people without diabetes.[34] The prevalence of coronary artery disease in patients with type 1 or 2 diabetes are widely different.[35][36] In the EURODIAB IDDM Complication Study which involved 3250 type 1 diabetic patients from 16 countries, the prevalence of cardiovascular disease was 9% in men and 10% in women; and it is increasing with age that it is 6% in the age group of 15–29 years and 25% in the age group of 45–59 years. In men, duration of diabetes was longer, waist-to-hip ratio greater, and hypertension more common in patients with cardiovascular disease, while in women, a greater body mass index was associated with increased prevalence of cardiovascular disease. The risk of coronary artery disease in type 1 diabetic patients increases dramatically when they have the onset of diabetic nephropathy.
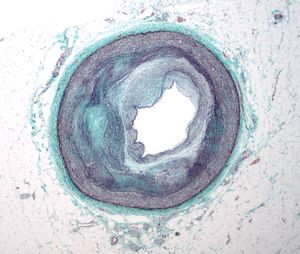
Diabetic men and women had comparable mortality rates, whereas coronary mortality among men was significantly higher.[37] Further evidences of the important relations between diabetes and myocardial infarction were obtained from the INTERHEART study in Canada. Diabetes increased the risk of myocardial infarction by more than two times in men and women, and independent of ethnicity. And thus a history of diabetes and myocardial infarction increased cardiovascular disease and mortality markedly. Diabetes or hyperglycemia itself and its complications are very important for the increased risk for coronary artery disease and related mortality.
Evaluation
Diabetes is commonly considered as a coronary artery disease risk equivalent. High-risk factors for coronary artery disease include: [38][39][40]
Typical or atypical symptoms
- 55 years of age or older
- Peripheral or carotid vascular disease
- And plus 2 or more of the following factors: hyperlipidemia, hypertension, smoking, family history of premature coronary artery disease, microalbuminuria, and progressive retinopathy.
Coronary artery disease is associated with smoking, diabetes, and hypertension. Limitation of blood flow to the heart by the artery may cause angina (chest pain) that occurs regularly with activity, after heavy meals, or at other predictable times due to microvascular dysfunction. Detection of coronary artery disease involves the usual diagnostic methods which include baseline electrocardiography (ECG), exercise stress testing ischemic ECG, myocardial perfusion scintigraphy, stress echocardiography, exercise radioisotope test (myocardial scintigraphy), coronary angiography, intravascular ultrasound and magnetic resonance imaging (MRI).
Treatments and outcomes
(Insert Table 12: ‘Treatment options based on accumulated evidence’, PMID17220161, p20) [38]
The preventive modalities include doctors counsel exercise, the “diabetes with CAD meal plan” aiming at long-term weight loss, aspirin in doses of 75 to 81 mg/d,[41] (in patients who do not tolerate or have a contra-indication to aspirin, clopidogrel can be used as an alternative antiplatelet agent [42]), antihypertensive therapy and glycemic control.
The optimization of glycemic control is important for prevention and control of any diabetes related cardiovascular diseases.[7] In addition to controlling cardiovascular risk factors, patients with diabetes should aim for good glycemic control (HbA1C < 53 mmol/mol or < 7% for all patients and, for the individual patient, an HbA1C as close as to normal (< 42 mmol/mol or < 6%) as possible) soon after the diagnosis of diabetes to prevent macrovascular as well as microvascular complications. Glycemic targets should be individualized according to the diabetes progression, comorbidities development, and the avoidance of the side effects of therapy (hypoglycemia and weight gain).
There is no simple and effective treatment for coronary artery disease currently. Therapeutic options are based on three principles:[43] 1) Medical treatment – medications like cholesterol lowering medications, beta-blockers, nitroglycerin, calcium antagonists, etc.; 2) Coronary interventions as angioplasty and coronary stent-implantation; 3) Coronary artery bypass grafting (CABG - coronary artery bypass surgery). Recent research progress focuses on new angiogenic treatment modalities (angiogenesis) and various stem cell therapies.
Heart failure and diabetes
Case Report
The 56-year-old plumber Rick was taking medications from his physician to protect his heart and brain, and he felt fluid retention, breathlessness and fatigue most recently. His clinical checkup data were: random blood glucose 388 mg/dL (21.5 mmol/L), fasting glucose 334 mg/dL (18.5 mmol/L), HbA1C 121.8 mmol/L (13.3%, his HbA1C had steadily increased over the past 8 months), total cholesterol 147 mg/dL (8.2mmol/L), HDL 78 mg/dL (4.3 mmol/L), LDL 82 mg/dL (4.6 mmol/L), Trigs 75 mg/dL (4.1 mmol/L), blood pressure 168/98. His physician recommended a diet plan but he refused since he had fast food daily due to his job and he loved chocolates.
Three months ago while Rick was on anti-hypertension medications, had a fall when he was in hospital for severe ‘flu’. Further tests in hospital diagnosed that he had a severely reduced left ventricular ejection fraction and diabetic nephropathy.
Introduction
Prevalence of diabetes and heart failure are increasing exponentially worldwide [44]. Diabetes is well-known to increase the risk of heart failure independent of other traditional risk factors and ischemia. Most heart failure in people with diabetes results from coronary artery disease, and diabetic cardiomyopathy is only said to exist if there is no coronary artery disease to explain the heart muscle disorder.[45] Little is known about the prevalence of the combination of diabetes and heart failure. The most recent and extensive data on the prevalence of diabetes and heart failure are from the Reykjavi´k Study, showing that the prevalence of the combination of heart failure and diabetes is 0.5% in men and 0.4% in women, increasing with increasing age. Heart failure was found in 12% of those with diabetes compared with only 3% in individuals without diabetes.[46] Thus, there was a strong association between diabetes and heart failure. In the Framingham study, the incidence of heart failure was double among males and five times higher in females with diabetes during 18 years of follow-up, compared with patients free from diabetes,
Several clinical and experimental studies have shown that diabetes mellitus leads to functional, biochemical, and morphological abnormalities of the heart, independent of promoting myocardial ischemia, and some of these changes happen earlier in the natural history of diabetes.[44] Diabetes is an independent risk factor for heart failure, and promotes myocardial remodeling (a precursor of heart failure), and the mechanisms beyond ischemia that lead to the development of heart failure in individuals with varying degrees of impaired glucose homeostasis. The most common abnormality observed in asymptomatic diabetics is left ventricular diastolic dysfunction, likely resulting from greater left ventricular myocardial and vascular stiffness. There is also growing evidence that some, if not all, of these structural and biochemical myocardial abnormalities start at the pre-diabetic stage.
(Insert Figure ‘Heart Failure’ from: http://en.wikipedia.org/wiki/Heart_failure )
Evaluation
The diagnosis of heart failure can be difficult, especially in the early stages. Although symptoms bring patients to medical attention, many of the symptoms of heart failure are non-specific and do not, therefore, help discriminate between heart failure and other problems. Symptoms that are more specific (i.e. orthopnea and paroxysmal nocturnal dyspnea) are less common, especially in patients with milder symptoms, and are therefore insensitive.[47] The echocardiogram and ECG are the most useful tests in patients with suspected heart failure. The echocardiogram provides immediate information on chamber volumes, ventricular systolic and diastolic function, wall thickness, and valve function. The ECG shows the heart rhythm and electrical conduction, i.e. whether there is sinoatrial disease, atrio-ventricular block, or abnormal intra-ventricular conduction. The ECG may also show evidence of left ventricular hypertrophy or Q waves (indicating loss of viable myocardium), giving a possible clue to the etiology of heart failure.
Routine biochemical and hematological investigations are also important to determine whether renin–angiotensin– aldosterone blockade can be initiated safely for renal function and potassium, to exclude anemia which can mimic or aggravate heart failure, and to provide other, useful information. Natriuretic peptide levels and Chest X-ray can be applied as references.
Treatments and outcomes
(Insert Table: ‘Heart failure and diabetes’, PMID17220161, p25) [38]
According to the European Society of Cardiology (ESC) and the European Association for the Study of Diabetes (EASD) Guidelines,[35] there are very few clinical trials on heart failure treatment specifically for diabetic patients. Information on treatment efficacy of various drugs is therefore based on diabetic subgroups included in various heart failure trials. A disadvantage of this is that the subgroups are not always well defined as regards the diabetic state and treatment. Most data favor a proportionately similar efficacy in patients with and without diabetes. Traditional treatment of heart failure in diabetic patients is based on diuretics, ACE-inhibitors, and Beta-blockades, as outlined in other guidelines.[48] Moreover, it is assumed that meticulous metabolic control should be beneficial in heart failure patients with diabetes.
Diuretics are mandatory for relief of symptoms that are due to fluid overload. These drugs should, however, not be used in excess since they induce neuro-hormonal activation.[48] ACE-inhibitors are beneficial in moderate-to-severe heart failure with and without diabetes, they inhibit angiotensin-converting enzyme, thereby decreasing the tension of blood vessels and blood volume, thus lowering blood pressure. Frequently prescribed ACE inhibitors include perindopril, captopril, enalapril, lisinopril, and ramipril. Hypoglycaemia has been reported following the institution of ACE-inhibitors in patients with diabetes on glucose-lowering treatment.[49] It is therefore recommended to monitor blood glucose carefully in the early phase of the institution of an ACE-inhibitor in such patients. Beta-blockade decreases myocardial free fatty acid exposure, thereby changing that metabolic pathway in type 2 diabetes.[50] The addition of eplerenone, a selective aldosterone blocker, to optimal medical therapy reduces morbidity and mortality among patients with acute myocardial infarction complicated by left ventricular dysfunction and heart failure.[51]
Atrial fibrillation and diabetes
Introduction
Evidences show that, apart from coronary artery disease, diabetic patients are at increased risk of arrhythmias.[55] The underlying risk factors for an arrhythmogenic substrate in patients with diabetes include imbalance in autonomic tone, silent ischemia, slowed conduction, heterogeneities in atrial and ventricular repolarization, and the extent of myocardial damage and scar formation.
Atrial fibrillation is relatively common in type 2 diabetes and is associated with substantially increased risks of death and cardiovascular events in patients with type 2 diabetes.[55] This arrhythmia identifies individuals who are likely to obtain greater absolute benefits from blood pressure-lowering treatment. Atrial fibrillation in diabetic patients should be regarded as a marker of particularly adverse outcome and prompt aggressive management of all risk factors. Atrial fibrillation is commonly observed in diabetic patients with prevalence rates estimated to be at least double than those among people without diabetes, and up to three times higher in patients with coexistent hypertension.[56]
Treatments and outcomes
(Insert Table: ‘Arrhythmias: atrial fibrillation…’, PMID17220161, p26) [38]
Aspirin and anticoagulant use as recommended for patients with atrial fibrillation should be rigorously applied in diabetic patients with atrial fibrillation to prevent heart stroke. Oral anticoagulation is most beneficial for patients at higher risk for stroke, whereas the risks outweigh the benefit in patients at low risk.[57] Thus, quantifying the risk of stroke is crucial for determining which atrial fibrillation patients would benefit most from anticoagulant therapy.
Based on the CHADSVASC risk score, all patient with diabetes and atrial fibrillation have an indication for anti-coagulation.[58]
Diabetic patients have a higher incidence of cardiac arrhythmias, including ventricular fibrillation and sudden death. The causes underlying the increased vulnerability of the electrical substrate in these patients are unclear and it is likely to be the consequence of the interplay of several concomitant factors. (i) Atherosclerosis [59] and (ii) microvascular disease [60] are increased in patients with diabetes and they concur to the development of ischemia that pre-disposes to cardiac arrhythmias. (iii) Diabetic autonomic neuropathy [61][62] leads to abnormal reflexes and innervation of the diabetic heart influencing electrical instability. (iv) The electrocardiogram of diabetic patients presents repolarization abnormalities manifesting as prolonged QT interval and altered T waves [62] that may reflect abnormal potassium currents.[63]
Microvascular disease and nephropathy are indicators of increased risk of sudden cardiac death in diabetic patients and should be under well controlled.
Control of glycaemia even in the pre-diabetic stage is important to prevent the development of the alterations that pre-dispose to sudden cardiac death. Microvascular disease and nephropathy are indications of increased risk of sudden cardiac death in diabetic patients.
Peripheral and cerebrovascular diseases and diabetes
Case Report
Simone is a 72-year old lady. She could not remember when she was diagnosed of type 2 diabetes. In one afternoon, while she was eating her late lunch with her husband, he noticed that she was no longer answering his questions and her lower jaw is slightly misplaced. Her husband tried to put on some cold packs to somehow soften the hardened jaw part but it didn’t work. So he drove her to the local hospital for check-up, but her doctor ordered for admission immediately.
As the consequence, Simone was diagnosed with an embolic stroke and atrial fibrillation at the time of admission. A few days after admission, Simone was getting worse. She could hardly speak and open her eyes, and was unable to swallow fluids. Her doctor had to order nasogastric tube insertion and oxygen administration. Her vital signs were: body temperature of 37.2 degree Celsius, blood pressure of 142/94 mmHg, pulse rate of 84 beats per minute of irregular rhythm, and respiratory rate of 24 cycles per minute. She looked generally weak and did not respond to questions, and not even to painful stimuli, and she elicited rates and crackling sounds during respiration, and was diagnosed of type 2 diabetes with emblic stroke with hemorrhagic conversion.
Introduction
Diabetes related peripheral and cerebrovascular diseases are peripheral vascular disease and stroke. Peripheral vascular disease (PVD, also known as peripheral artery disease, PAD) is a term used to refer to atherosclerotic blockages found in the lower extremity, and it causes either acute or chronic ischemia (lack of blood supply). It has a two- to four-fold increased incidence in subjects with diabetes, which is present in 15% of diabetic patients. The ankle/brachial systolic blood pressure index, a noninvasive measure of peripheral vascular disease, is widely used in epidemiological studies.[64][65] The symptomatic manifestations of peripheral vascular disease are intermittent claudication and limb ischemia. Impairment of the circulation in the foot owing to diabetic macro- and microvascular diseases is the most common non-traumatic reason for limb amputation. The prevalence of peripheral vascular disease increases with advancing age, duration of diabetes, and peripheral neuropathy. The latter condition may mask the symptoms of limb ischemia and thus disease progression may be advanced before patients and healthcare providers realize that peripheral vascular disease is present. About 20% of patients with mild peripheral vascular disease may be asymptomatic; other symptoms include:[66]
- Claudication like pain, weakness, numbness, or cramping in muscles
- Sores, wounds, or ulcers that heal slowly or not at all
- Noticeable change in color or temperature when compared to the other limb, or to both limbs
- Diminished hair and nail growth on affected limb and digits.
Cerebrovascular disease is a group of brain dysfunctions related to problematic blood vessels supplying the brain, and hypertension is the most important cause.[67] The typical cerebrovascular disease in diabetes is brain stroke, which is the second leading cause of death worldwide. A transient ischemic attack (minor stroke) leaves little to no permanent damage in the brain, which symptoms include facial weakness, visual impairment, loss of coordination or balance, sudden headache, and mental confusion with unintelligible speech. And symptoms of a cerebral contralateral (opposite sided) include paralysis of a single body part; paralysis of one side of the body; localized tingling, numbness; hemianopia visual loss; aphasia (loss of speech); even loss of consciousness.
Cerebrovascular mortality rates have been shown to be raised in patients with type 2 diabetes and have been reported that it is at least as great a risk factor in type 1 diabetes as in type 2. It is found that cerebrovascular mortality is raised at all ages in these patients.[68] Typical brain strokes can be classified into two categories: ischemic and hemorrhagic strokes.[67] Ischemic strokes are those that are caused by vessel occlusion mostly by embolism, while hemorrhagic strokes (intracerebral hemorrhage) are the ones which result from rupture of a blood vessel due to hypertension. About 80% of strokes are caused by ischemia, and the remainder by hemorrhage. Some hemorrhages develop inside the areas of ischemia, and thus it is unknown how many hemorrhages actually start as ischemic stroke.
(image: http://commons.wikimedia.org/wiki/File:Bluthirnschranke_nach_Infarkt_nativ_und_KM.png)
Evaluation
Peripheral vascular diseases: An objective measure of peripheral vascular disease is the ankle–brachial blood pressure index, defined as the ratio between the arterial pressure at the ankle level and in the brachial artery with the highest pressure,[64] which means that when the blood pressure reading in the ankles is lower than that in the arms, blockages in the arteries providing blood from the heart to the ankle are suspected. The ankle–brachial blood pressure index should normally be 0.9. This measurement is valuable for early detection of peripheral artery disease and also for a better stratification of overall cardiovascular risk. A 0.5 or an ankle pressure as 50 mm Hg indicates severely impaired circulation to the foot, below 0.8 indicates moderate ischemic disease, and below 0.5 implies severe ischemic disease, alternatively a 0.4 is used as a threshold. An index above 1.3 indicates poorly compressible vessels as a result of stiff arterial walls, which in diabetic patients are due to atherosclerosis in the media layer of the arterial wall.
Further traditional examinations include a lower limb Doppler ultrasound, an angiography where a catheter is inserted into the common femoral artery and selectively guided to the artery, or an X-ray by injecting a radio dense contrast agent to observe the artery directly. On the other hand, modern and non-invasive technologies like multislice computerized tomography (CT) scanners and magnetic resonance imaging (MRI) provide direct imaging of the aorta and lower limb arteries without the need for an injection of contrast agents and as an alternative to angiography.
Cerebrovascular diseases: After transient ischemic attack or minor stroke, the risk of further stroke is substantially higher than previously thought, reaching as high as 30% within the first month in some subgroups.[67] Patients at very high risk (>30%) of recurrence within 7 days can be identified on the basis of their ages, blood sugar levels, blood pressures, and other symptoms. Simple risk scores have been developed on the basis of these factors to predict those patients at greatest risk who might benefit the most from early risk-factor modifications.
Both the ischemic and hemorrhagic strokes are diagnosed through the following techniques: a neurological body examination, Doppler ultrasound, arteriography, and CT and MRI scans of the brain. The imaging techniques will assist in determining the subtypes and causes of stroke. And blood tests may be helpful in finding out the causes of stroke.
Treatments and outcomes
(Insert Table: ‘Peripheral vascular disease’, PMID17220161, p29) [38]
(Insert Table: ‘Stroke’, PMID17220161, p31) [38]
Peripheral vascular diseases: Preventions are most important strategies, such as regular exercises, the optimization of glycemic control, management of hypertension, smoking cessation, antiplatelet and anti-cholesterol medications like aspirin, clopidogrel and statins.
For diabetic patients with peripheral vascular disease, general measures to reduce overall cardiovascular risk should be intensive, and treatment of hypertension should be vigorous. But in patients with critical limb ischemia and very low distal perfusion pressures, it may be dangerous to lower blood pressure too much for the foot, and thus blood pressure should be kept at a level permitting adequate arterial inflow to the distal extremity. Platelet inhibition with low-dose aspirin, in the magnitude of 75–250 mg per day, is indicated in all patients with severe peripheral vascular disease; further inhibition of platelet aggregation by clopidogrel or dipyridamole along with anticoagulation with low molecular weight heparin may be the first set of choice.[28][29][32]
If anatomically possible, a revascularization procedure should be attempted in all patients with critical limb ischemia,[30] such as an angioplasty or a bypass grafting can be done on solitary lesions in large arteries like the femoral artery, but the revascularization may not have sustained benefits. A synthetic prostacyclin (Ilomedin, Iloprost) is the only pharmacological agent so far convincingly shown to have significant beneficial effects on ulcer healing and pain relief on patients with critical limb ischemia, which is given intravenously daily for a period of 2–4 weeks.[31]
Cerebrovascular diseases: Stroke prevention should be based on a multifactorial strategy aimed at the treatment of hypertension, hyperlipidemia, microalbuminuria, hyperglycemia and the use of antiplatelet medications. Antiplatelet therapy reduces the incidence of stroke in diabetic patients and is indicated for both primary and secondary prevention.[69] Low dose Aspirin (75–250 mg daily) should be the initial choice, but in case of intolerance, clopidogrel 75 mg once daily should be given.[70] In patients with recurrent stroke, a combination of aspirin and dipyridamol should be a better option.
After a transient ischemic attack or stroke, since complications are more frequent in diabetic subjects compared with non-diabetic subjects, special attention should be paid to the overall risk for peri- and post-operative morbidity and mortality when making decision on surgical interventions, and a simple risk score that can be used to stratify patients into different risk groups for complications after surgery has been developed.[71] An alternative to endoarterectomy is carotid artery angioplasty and carotid artery stenting, which has been found to be not inferior to endoarterectomy and may prove to be a preferable method in high-risk patients.[72]
The treatment in the acute phase of stroke in diabetic patients should follow the same principles as in the general population, and patients should be kept in stroke care units as the routine management to close surveillance of vital functions and optimization of circulation and metabolic conditions.[67]Thrombolysis like recombinant tPA is one of the most effective treatments but requires application within 3–4 h of stroke onset, which reduces mortality and disability from stroke, but is associated with a risk of hemorrhage. Because of the substantial effectiveness of tPA, efforts to increase the number of patients who are eligible for thrombolytic therapy, and combination of tPA with modern imaging technologies are underway.[67] Hemispheric decompression in young patients with malignant middle cerebral artery territory infarction and space occupying brain edema is supported by evidence. Mechanical thrombectomy and hemicraniectomy could be other options.[73][74]
As reviewed recently, strict blood glucose control with intensive insulin therapy improved mortality and morbidity of adult diabetic stroke patients. Besides saving lives, intensive insulin therapy largely prevented several critical illness-associated complications including critical illness polyneuropathy, blood stream infections, anemia, and acute renal failure.[75] But arguments of the safety of the intensive insulin therapy on diabetic patients are ongoing, and new evidences show that diabetic critical-ill patients react differently to the therapy compared to non-diabetic ones, and a carbohydrate-restrictive strategy could be safer and as efficient as intensive insulin therapy, and thus could be a replacement in the near future.[76][77]
References
Error fetching PMID 10413697:
Error fetching PMID 17192512:
Error fetching PMID 17353438:
Error fetching PMID 430798:
Error fetching PMID 20609967:
Error fetching PMID 9686693:
Error fetching PMID 16194123:
Error fetching PMID 20200384:
Error fetching PMID 12502659:
Error fetching PMID 12876091:
Error fetching PMID 15662552:
Error fetching PMID 12610023:
Error fetching PMID 16305061:
Error fetching PMID 16210931:
Error fetching PMID 12687329:
Error fetching PMID 11832527:
Error fetching PMID 14632698:
Error fetching PMID 12719277:
Error fetching PMID 11315831:
Error fetching PMID 14706054:
Error fetching PMID 11772915:
Error fetching PMID 11874956:
Error fetching PMID 15793191:
Error fetching PMID 10331395:
Error fetching PMID 11023146:
Error fetching PMID 8799621:
Error fetching PMID 15364185:
Error fetching PMID 17220161:
Error fetching PMID 10749967:
Error fetching PMID 17291928:
Error fetching PMID 17488967:
Error fetching PMID 17506599:
Error fetching PMID 22108732:
Error fetching PMID 15094099:
Error fetching PMID 15735197:
Error fetching PMID 22828712:
Error fetching PMID 15901669:
Error fetching PMID 9283780:
Error fetching PMID 12106931:
Error fetching PMID 12668699:
Error fetching PMID 19282274:
Error fetching PMID 16274775:
Error fetching PMID 10507957:
Error fetching PMID 22922413:
Error fetching PMID 7867189:
Error fetching PMID 9484982:
Error fetching PMID 18468545:
Error fetching PMID 12574553:
Error fetching PMID 8918275:
Error fetching PMID 11372014:
Error fetching PMID 12941721:
Error fetching PMID 10666287:
Error fetching PMID 7525794:
Error fetching PMID 9243111:
Error fetching PMID 8981292:
Error fetching PMID 14526040:
Error fetching PMID 16476626:
Error fetching PMID 22182267:
Error fetching PMID 21190097:
Error fetching PMID 19531590:
Error fetching PMID 21871056:
Error fetching PMID 19327317:
Error fetching PMID 16399854:
- Error fetching PMID 117544:
- Error fetching PMID 10413697:
- Error fetching PMID 17192512:
- Error fetching PMID 17353438:
- Error fetching PMID 430798:
- Error fetching PMID 20609967:
-
DeFronzo RA. International Textbook of Diabetes Mellitus. 3rd ed. Chichester, West Sussex; Hoboken, NJ: John Wiley; 2004.
- Error fetching PMID 9686693:
- Error fetching PMID 16194123:
- Error fetching PMID 20200384:
- Error fetching PMID 12502659:
- Error fetching PMID 12876091:
- Error fetching PMID 15662552:
- Error fetching PMID 12610023:
- Error fetching PMID 16305061:
- Error fetching PMID 16210931:
- Error fetching PMID 12687329:
- Error fetching PMID 11832527:
- Error fetching PMID 14632698:
- Error fetching PMID 12719277:
- Error fetching PMID 11315831:
- Error fetching PMID 14706054:
- Error fetching PMID 11772915:
- Error fetching PMID 11874956:
- Error fetching PMID 12574553:
- Error fetching PMID 8918275:
- Error fetching PMID 12941721:
- Error fetching PMID 10666287:
- Error fetching PMID 11372014:
- Error fetching PMID 15793191:
- Error fetching PMID 10331395:
- Error fetching PMID 11023146:
- Error fetching PMID 8799621:
- Error fetching PMID 15364185:
- Error fetching PMID 17220161:
- Error fetching PMID 10749967:
- Error fetching PMID 17291928:
- Error fetching PMID 17488967:
- Error fetching PMID 17506599:
-
Jameson JN, Kasper DL, Harrison TR, Braunwald E, Fauci AS, Hauser SL, Longo DL. Harrison's Principles of Internal Medicine (16th edition). 2005. New York: McGraw-Hill Medical Publishing.
- Error fetching PMID 22108732:
- Error fetching PMID 15094099:
- Error fetching PMID 15735197:
- Error fetching PMID 22828712:
- Error fetching PMID 15901669:
- Error fetching PMID 9283780:
- Error fetching PMID 12106931:
- Error fetching PMID 12668699:
-
Shoback, edited by David G. Gardner, Dolores (2011). Greenspan's basic & clinical endocrinology (9th ed.). New York: McGraw-Hill Medical. pp. Chapter 17. ISBN 0-07-162243-8
- Error fetching PMID 16399854:
- Error fetching PMID 19282274:
- Error fetching PMID 16274775:
- Error fetching PMID 10507957:
- Error fetching PMID 22922413:
-
pmid=A
-
pmid=B
-
pmid=C
-
pmid=D
-
pmid=E
-
pmid=F
- Error fetching PMID 7867189:
- Error fetching PMID 9484982:
- Error fetching PMID 18468545:
- Error fetching PMID 7525794:
- Error fetching PMID 9243111:
- Error fetching PMID 8981292:
- Error fetching PMID 14526040:
- Error fetching PMID 16476626:
- Error fetching PMID 22182267:
- Error fetching PMID 21190097:
- Error fetching PMID 19531590:
- Error fetching PMID 21871056:
- Error fetching PMID 19327317: